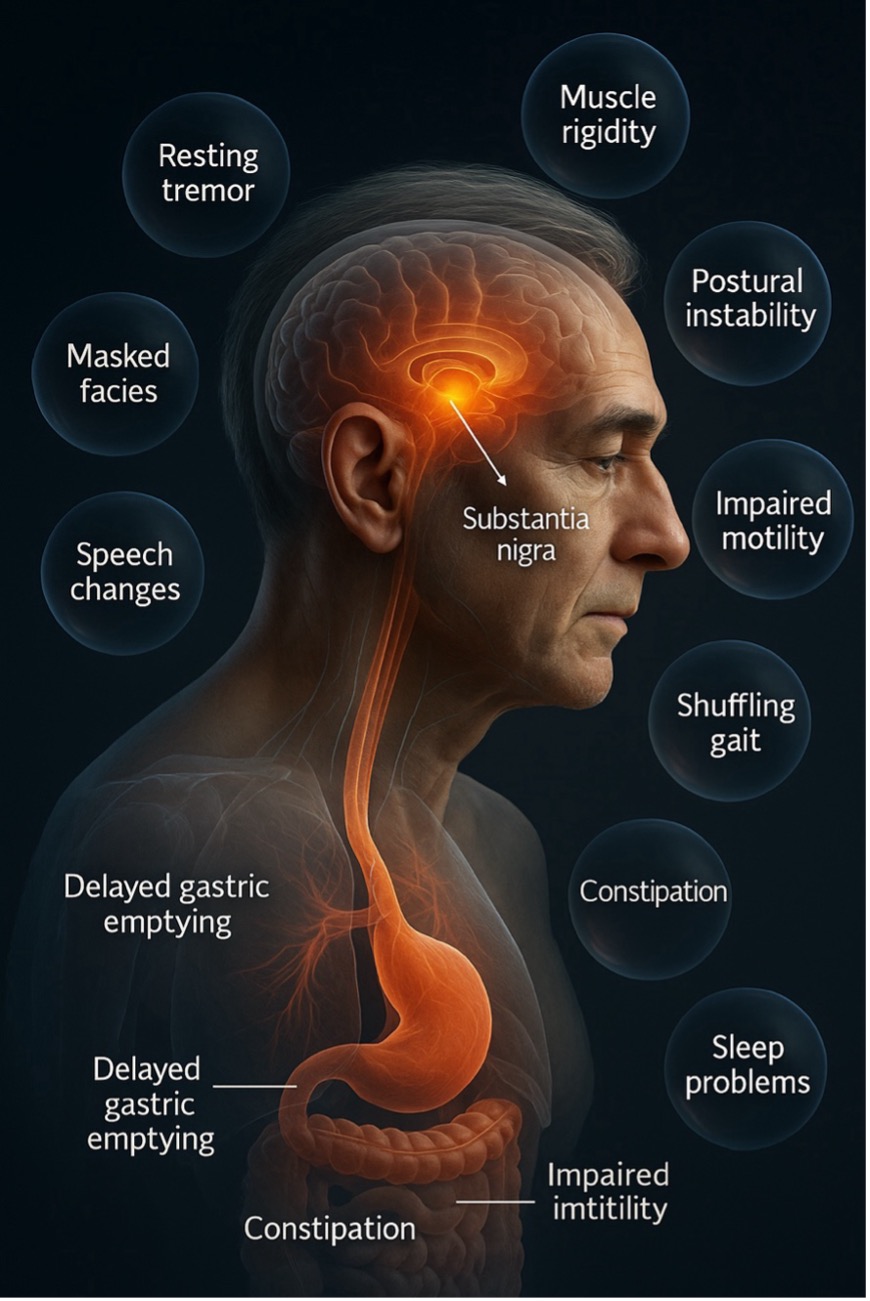
Parkinson’s disease (PD) is a complex, progressive neurological condition that affects movement, balance, mood and many non-motor functions. While there is no cure, a growing body of clinical research and lived experience shows that regular physical activity, a supportive environment and appropriate lifestyle choices can substantially improve motor performance, mood, quality of life and even the day‑to‑day effectiveness of medication. This chapter summarizes the main benefits people with Parkinson’s can gain from exercise in general, explains why outdoor and water‑based sports have particular advantages, reviews the positive role of warm sunny environments, and outlines how a Mediterranean (especially Greek) diet and good intestinal transit support overall care. It ends with a personal account of living well with PD through kite surfing and a practical invitation to explore these options safely.
Why every person with Parkinson’s should practice regular physical activity
Exercise is medicine. For people with PD, studies consistently show that regular, appropriately tailored physical activity:
– Improves gait, balance, strength and flexibility, reducing risk of falls and improving independence.
– Reduces brady-kinesia (slowness) and rigidity and helps maintain range of motion.
– Enhances mood, reduces anxiety and depression, and boosts self‑confidence and social engagement.
– Promotes cardiovascular fitness and general health, which are important for long‑term outcomes.
– Supports neuro-plasticity — exercise stimulates molecular and cellular processes (including increases in growth factors) that help the brain adapt and optimize remaining pathways.
Because PD affects each person differently, exercise programs should be individualized and progressed with professional guidance (neurologist, physiotherapist, PD nurse or certified exercise instructor). Still, the overall evidence supports making exercise a core component of PD management from the time of diagnosis.
Added benefits of exercising outdoors
Outdoor exercise amplifies many of the benefits of physical activity. Reasons include:
– Sunlight exposure increases vitamin D production, which supports bone health, muscle function and mood regulation. Vitamin D deficiency is common in older adults and has been linked to worse motor outcomes.
– Fresh air and natural settings reduce stress and improve mood and cognitive clarity through documented psychophysiological mechanisms.
– Outdoor movement often involves larger, more variable motor patterns (walking on sand, balancing on a board) that challenge coordination and balance beneficially.
– Social opportunities and a sense of freedom outdoors increase adherence — people are more likely to keep doing activities they enjoy.
Why water sports can be particularly valuable for people with Parkinson’s
Water sports — such as kite surfing, wing foiling, kite foiling, paddle-boarding and therapeutic aquatic exercise — offer several distinct advantages for many people with PD:
– Water reduces joint loading and the risk of impact injuries, allowing vigorous exercise without excessive stress on knees, hips and spine.
– Balance training with reduced fear of falling and improve body condition.
– Whole‑body engagement: Water sports recruit core, postural and limb muscles in dynamic ways that improve coordination and functional strength.
– Rapid engagement and reward: The immediate feedback and thrills of watersports can produce strong positive emotional responses that motivate continued practice.
These features make water sports a powerful option for many people with PD who can safely participate, especially when coached by instructors with experience working with neurological conditions.
Warm, sunny weather—physiological and psychological benefits
Spending time in warm, sunny climates adds benefits beyond the activity itself:
– Warmth reduces muscle stiffness and can make movement feel easier.
– Sunlight regulates circadian rythms and can improve sleep quality, which is crucial for motor and non‑motor symptom control.
– Better mood and reduced stress in pleasant climates support motivation and resilience.
Hydration and sun safety are important considerations; but for many people with PD, a warm, sunny environment supports more comfortable and sustained activity.
Mediterranean and Greek food: why it helps
The Mediterranean diet — abundant in vegetables, fruits, whole grains, fish, olive oil and moderate dairy — is associated with improved cardiovascular health, lower inflammation and better cognitive outcomes compared with typical Western diets high in processed foods, added sugars and saturated fats. Greek cuisine often exemplifies these principles and tends to be high in fresh vegetables, fruits, olive oil and fish.
Key benefits relevant to PD include:
– High fiber intake supports regular intestinal transit. Constipation is a common and early problem in PD and can worsen quality of life and complicate medication timing.
– A diverse, rich in fiber diet supports a healthier gut microbiome; emerging evidence links gut health to brain health and symptom expression in PD.
– Lower consumption of ultra‑processed foods reduces systemic inflammation that can worsen overall health.
Compared with many standard European or American diets that are higher in processed foods and lower in fiber, a Mediterranean/Greek diet typically produces more regular bowel function and a gut environment supportive of medication absorption and general well‑being.
Intestinal transit, medication effectiveness and Parkinson’s
Many PD medications (notably levodopa) require predictable absorption in the gut to work optimally. Gastrointestinal dysmobility, delayed gastric emptying and constipation — all common in PD — can delay or reduce medication absorption, causing fluctuations in symptom control. Maintaining regular bowel habits through diet, hydration, physical activity and medical management when needed helps stabilize medication response and daily function.
How activity influences adrenaline and dopamine and why that matters
Physical activity triggers short‑term increases in catecholamines (adrenaline/epinephrine) that enhance alertness and motor readiness. Repeated exercise also promotes dopamine neurotransmission and supports neuroplasticity through growth factors (such as BDNF). For people with PD — who have impaired dopamine signaling — these activity‑driven effects can translate into improved movement, motivation and mood both immediately (a better “on” period) and over the longer term through adaptive changes in the brain.
A lived example: kite surfing and life with Parkinson’s
I was diagnosed with Parkinson’s disease in 2015. Since then, kite surfing has become a central part of my life. I now spend many hours per day, eight months a year, kite surfing and related water activities. These experiences have helped me regain confidence, reduce symptoms during active periods, improve balance and fitness, and reclaim a sense of freedom and joy.
If you are recently diagnosed, I warmly encourage you to consider visiting Greece to try kite surfing under experienced supervision. Surfing Bird kite school and its team have long experience teaching and supporting kite surfing, kite foiling, wing foiling and SUP. Their safety team watches closely and can detect early signs of an off‑phase and promptly assist with a boat rescue if needed. The instructors understand the challenges of learning a complex sport while living with PD and adapt teaching and safety to your needs. Exercise, a supportive outdoor environment, water sports and a Mediterranean diet form a powerful, complementary approach to improving daily life with Parkinson’s disease. While individual responses vary and nothing replaces medical care, many people living with PD consider that these elements together accelerate functional gains, stabilize medication effects and restore a sense of possibility and joy. If you are newly diagnosed, consider exploring these options with professional guidance — and, if appropriate, experience the unique combination of sea, sun and skilled instruction kite surfing in Greece offers.